You Don’t Need to Always Have “Obesity” to Benefit from Expert Help
One of the most common questions I hear is: “My BMI is normal—can you still help me?”
The short answer? Absolutely.
At Weight Sense, we understand that the number on your BMI chart doesn’t tell the whole story. Even patients with “normal” BMI who are concerned about their weight can benefit tremendously from a comprehensive, 360-degree review of their health and lifestyle to determine the next best steps to improve their health and wellneing. Especially when risks of weight-related metabolic health risk is present such as fatty liver disease, high blood pressure or diabetes.
Why Normal BMI Doesn’t Mean “Nothing to Worry About”
BMI is just one metric—and it’s far from perfect. Here’s what really matters:
Body Composition Matters More Than BMI
Two people can have the same BMI but completely different body compositions. That’s why we measure body composition to understand what’s really happening beneath the surface. If you don’t have access to an InBody like we do in clinic, you can go to Inbody.com and find a testing site near you. Even at a BMI less than 25, an individual can have higher percent body fat. There are also ethnic variations in terms of weight health that matter too.
Significant Weight Gain Over Time
A 10% total body weight gain over 1-2 years is concerning to me, even in someone with “normal BMI.”
For example, if you’ve gone from 140 pounds to 160 pounds, that’s a yellow flag worth investigating.
Generally, regular exercise would halt this kind of weight gain—so when it doesn’t, we need to look deeper and to come up with a plan to stop the weight gain and initiate weight loss.
Your Metabolic Health
Metabolic health conditions are a critical part of the weight biology overview. The presence of conditions like fatty liver disease, heart disease, type 2 diabetes, high blood pressure, obstructive sleep apnea (OSA), or Polycystic Ovary Syndrome (PCOS) fundamentally alters how your body manages weight and energy. These conditions are deeply intertwined with metabolic function, and their presence is a significant factor we review when assessing how your weight affects your health—even for those with a “normal” BMI. Ignoring these metabolic red flags based solely on a BMI number is a mistake. Our focus is on treating the underlying biology, not just the scale or one metric.
Real Cases From My Practice This Week
Let me share some examples of patients I saw just this week—all with different stories, but all benefiting from specialized weight care and a plan to improve their health.
Case 1: The Asian American Patient with Hypertension
A woman in her mid 40s with a BMI 25 with high blood pressure. She had been trying to lose weight with very low calories and omitting carbs but felt exhausted. She had no energy. My first priority? Getting them feeling better and eating properly again. Checking labs and med list to investigate further. We reviewed her meals, I recommended adding in complex carbs for energy and we monitored her body composition changes over one month. She came back after the holidays for follow up visit and gained muscle mass, reduced body fat and felt better.
Case 2: The Midlife Woman
Despite eating a whole-foods diet and doing HIIT workouts 5 days a week, this patient experienced a 20-pound weight gain that continues to climb. She has a family history of obesity and is now in midlife, both significant factors that require medical evaluation. Given risks factors, ethnic variations in BMI and her healthful lifestyle, we determined trying a medication to improve her health would be beneficial.
Case 3: Normal BMI with Fatty Liver Disease
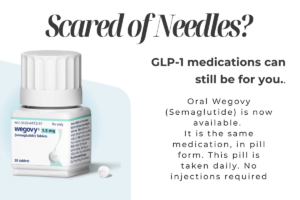
This patient had completely normal BMI but developed fatty liver disease—a serious metabolic condition that needs intervention regardless of what the scale says. Body composition showed high percent body fat. She also did not like the idea of injections. So we discussed Wegovy Pill.
What We Look For: The Variables That Matter
When someone comes to see me concerned about their weight, I conduct a thorough investigation. Here’s what we explore together:
✓ Lifestyle optimization – Can we improve sleep, stress management, or activity levels?
✓ Medications – Are you on a weight-promoting medication that needs adjustment?
✓ Exercise barriers – Did you stop exercising because you weren’t seeing weight loss?
✓ Hormonal changes – Is menopause playing a role?
✓ Metabolic factors – Do you have a “hungry brain” or metabolic dysfunction?
✓ Sleep quality – Are you getting adequate, restorative sleep?
✓ Weight-related medical issues – Sleep apnea, atherosclerosis, fatty liver, or other conditions
Ready to Take the Next Step?
If you’re concerned about your weight or metabolic health—even with “normal” BMI we’re here to help. Contact Weight Sense today to schedule your comprehensive evaluation.
Because your health deserves more than a one-size-fits-all approach.
Dr. Nikita Shah, DO, DABOM
Board-Certified Obesity Medicine Physician
Founder & CEO, Weight Sense
Lake Nona, Orlando, Florida
407-753-5036
Wanna get your head in the game?
Check out this fantastic post and conversation with Dr. Rashmi Schramm about understanding the Mind-Body Connection. Jump to it by clicking here:
https://weight-sense.com/train-your-mind-for-success-understanding-the-mind-body-connection/